I wrote earlier this year about some injuries sustained in the Spencer household and our plans to manage them conservatively, at least without immediate surgery. The original piece is here: Doubling Down on Non-surgical Conservative Care.
In a short period of time last winter, Kate had sustained a knee injury and I had a mallet thumb injury (extensor pollicis longus rupture). If we had sought formal medical consultation, surgery most certainly would have been recommended for each. In fact, for my thumb injury, I did casually consult an Orthopedic surgeon who did recommend surgery. I work closely with and respect this surgeon greatly. He did a sort of magic trick – before asking me what happened, he took a look at my x-ray and said, “You can’t extend your thumb, can you?” Magic. Impressive. Brilliant Doctor. But, I ignored his advice, “You’ll likely do better with surgery than without. If it were my thumb, I’d have the surgery.” The contention was that the tediousness and fragility of daily splinting routine sometimes leads to failure with conservative management. The surgical procedure would not repair the torn extensor tendon, but it would better immobilize the thumb so that healing could occur in a more predictable fashion than with bracing. After reviewing the available literature, which was mostly case studies, I decided to take my chances and go with the daily splinting. My expectation was that I would regain much of my thumb DIP extension, but likely come up 10 to 20 degrees short of full extension.
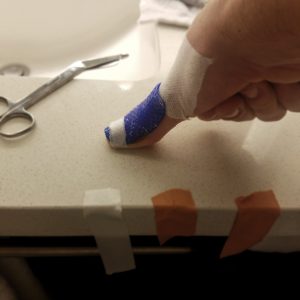
Here I am pressing my thumb into the counter to keep it extended while I work to re-tape and support it. I had to keep it extended on a surface while I washed it, dried it, and taped it daily.
8 weeks of splinting my thumb in hyperextension – untaping, washing, drying, and retaping every morning while passively maintaining extension. After all the splinting, it took another few months of recovery to regain motion and strength. Eventually, my results ended up being better than you’re supposed to get following a rupture of the EPL. There’s a little lag in extension, but I am able to actively hyperextend the thumb. I’ve come away with two conclusions about the conservative management of a mallet injury (thumb or finger) through my reading and through my personal experience:
- Early intervention is essential for successful conservative management. My OT co-workers had me splinted within 12 hours of the initial injury – research also indicates that success falls off after only 1 to 2 days if splinting is not initiated.
- Compliance, man. Compliance. A person with a mallet injury has to be fastidious about keeping the thumb extended while changing the bandages and occasionally cleaning the thumb. The rule is that if you accidentally bend the thumb, your 8 weeks of splinting starts over – I would contend that each time the thumb is accidentally bent, several degrees of active extension is lost forever. I have myself as a PT, my wife as a PT, and OTs/Certifed Hand Therapists as close friends… I figured I was a good candidate for being able to manufacture 8 weeks of compliance. For our patients, we need to educated them to a great extent on the importance of maintaining extension.
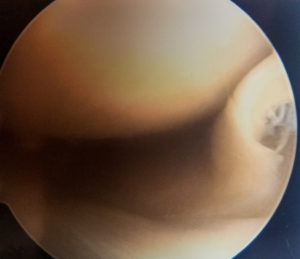
Here, on the far right side of the picture, is Kate’s flipped over bucket handle tear of her meniscus… see it?
Now, Kate’s story is a far more fascinating story that perhaps raises more questions than it gives answers to. While pregnant, she had sustained what I am convinced was an ACL injury. She was super-lax when I tested her Lachman’s on the day of the injury – a very, very late endfeel, lots of translation. Because she had her ACL previously reconstructed, I had actually tested her knee before the injury and knew the knee to be very stable. Because she was pregnant at the time of the injury, she made the decision to wait and see what the knee was like after pregnancy and after the hormones that goes along with pregnancy had passed. After she had the baby, she got an MRI to see what might be going on in her knee since it was feeling much better, but not perfect. The MRI showed some lateral meniscus damage and an ACL that existed but didn’t appear robust. The same Ortho that I saw for my thumb took a casual look at her MRI and commented that the posterior lateral corner damage may be a sign that “an anterior subluxing event may have occurred,” again, great info discerned from what could be interpreted as a fairly benign MRI. Anyways, by this point, the knee was testing more stable and never, ever giving Kate a feeling of giving out. The decision was made to continue with strengthening and conservative management. Over time, the knee felt well on a day-to-day basis. We hiked a fair amount this summer and Kate even got one late-November ski day in without any issue. Her knee was feeling pretty good… until she knelt down two weeks ago. Her knee swelled up and became an immediate problem. She continued to not have any feeling that her knee was giving out, but now it was stiff, swollen, and sore. After pushing through a race 3,000 ft up Aspen Mountain on the injured knee and with the end of the deductible year fast-approaching, Kate and Tom Pevny, an Orthopedist at Aspen Valley Hospital where we work, decided that scoping the meniscus and laying some eyes on the actual condition of the ACL seemed like a prudent plan. Though Kate still had some reservations going into the surgery about whether she really needed it, the surgery was justified when Dr. Pevny let her know that he had taken out a sizeable bucket-handle tear from the lateral meniscus. Had she left it alone, it certainly would have continued to give her troubles.
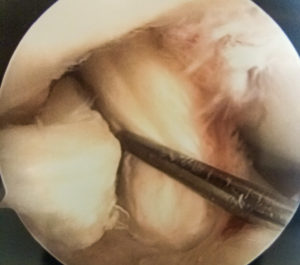
Here is Kate’s intact and robust ACL.
Now for the million dollar question: What about the ACL? Dr. Pevny says it looks good. The stability is that “of a typical reconstructed ACL”. Whenever Dr. Pevny does talks on the ACL, he emphasizes techniques that mimic replication of the anatomical footprint of the ACL and the ability of a well-performed reconstruction to stabilize the knee in various positions – this point is emphasized in his research papers as well. I get the impression that he believes Kate’s previous reconstruction to be adequate but not equivalent to what could be done today. I, on the other hand, believe that Kate’s reconstruction in ’94 was done extremely well, and that the knee was extraordinarily stable with a very tight ACL. I also believe that the ACL was stretched and loosened during her accident last winter. If this is true, that her ACL acquired some laxity, but within an acceptable range that still allows full function, I have a lot of questions that I don’t think current research answers. Did the presence of the hormone relaxin during Kate’s pregnancy actually allow her enough ligamentous laxity to avoid more a serious injury? Did the ACL remain stretched and then “reduce” more than it normally would have when the pregnancy hormones retreated? Does relaxin even act on a reconstructed ACL like it does on a native ligament? I would think it does. There’s a whole string of unanswerable questions that I find just fascinating. If you have any thoughts on my hypothesis and questions, or questions of your own, I’d love you to comment below…
So, in the end: a. My thumb is back to 98% of it’s original self through non-surgical care. b. Kate didn’t wholly avoid surgery, but her patience in waiting to see what the knee did following injury may have allowed her to avoid a long, protracted ACL recovery in exchange for a much quicker meniscal clean-up.
We, Physical Therapists and Occupational Therapists, are THE specialists in conservative management of orthopedic conditions. In circumstances where surgeons and patients are often far too trigger-happy to start cutting, we have to be the balancing voice that educates our clients on the benefits that a little patience and work may have on avoiding surgery which is and should always be the last resort.


